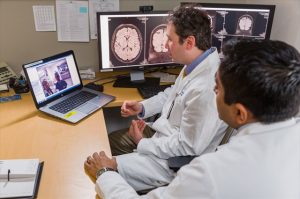
The next great technological disruption may be in health care and hints of this are just starting to appear in Fairfield County with the launching of telemedicine initiatives, also known as telehealth.
Medical networks are aiming to improve access to care, relieve the burdens on overwhelmed and understaffed facilities and reduce health care costs by connecting to patients via digital means.
“There is no question that telehealth is going to be something that we take for granted,” said John R. Patrick, author of “Health Attitude: Unraveling and Solving the Complexities of Healthcare” (2015, Attitude LLC).
“It might take a few years to get to that point, but it is emerging rapidly across the country,” said Patrick, a Fairfield County resident, who served as vice president of internet technology during his 35-year career at IBM before going on to focus his tech expertise on providing solutions to challenges in the health care industry ”“ the focus of his book.
Health care services that were traditionally found in hospitals and doctor”™s offices are now literally in the palms of patients through smartphones.
Specially designed phone attachments allow medical professionals to identify skin issues through high-resolution photos or to look inside the ear of a child with a suspected infection or conduct EKG tests, Patrick said.
“A year ago, the FDA approved 250 medical devices for use with smartphones,” he said.
But the spread of these advances in health care has not been even across the country, said Gene Buccini, a Western Connecticut State University professor of management specializing in health care.
“In other parts of the country you find it much more widespread than here.”
According to Buccini, telemedicine already has a foothold in Silicon Valley and parts of rural America where high levels of technology adoption and geographical barriers to treatment have spurred the use of video, photo and text to connect doctors and patients.
Virtual care has been somewhat slower in Fairfield County, said Dianne Auger, senior vice president and chief strategy officer at St. Vincent”™s Medical Center in Bridgeport.
“They call Connecticut the land of steady habits,” she said. “To break into the new world here is sometimes a little difficult, but I also think people are looking for innovation and once they try it they are hooked.”
At St. Vincent”™s, a telemedicine pilot program has been in use since this past winter and a full-scale service was just launched.
The hospital”™s new website, myvirtualcare.com, allows patients to be treated for common conditions such as sinus infections, female bladder infections, pink eye, or colds, coughs, and the flu for a set fee of $35 ”“ less than the cost of many insurance co-pays, the hospital noted.
By detailing their symptoms in an online interview form, patients are able to receive a diagnosis and treatment plan from a St. Vincent”™s health professional, typically in one hour. Treatment can include drug prescriptions, which are forwarded electronically to the patient”™s pharmacy and if urgent care is needed, staff can book an appointment or advise the patient to seek immediate emergency care.
The service is open seven days a week from 8:30 a.m. to 10 p.m.
Auger describes telemedicine as the next wave in on-demand care ”“ a spillover effect from the on-demand trend sweeping through segments of the economy led by Uber and Amazon and a sea of startup companies.
The wave began in health care with the rise of urgent care and walk-in clinics at places such as Walmart and CVS Health, as well as AFC Doctors Express Urgent Care in Fairfield County and the Northeast.
Beyond the altruistic philosophy of improving patient access to quality care, Buccini said cost-controlling changes in the industry”™s compensation model has been the primary factor in the shift toward virtual care.
Danbury Hospital and St. Vincent”™s are part of an industrywide transition from the fee-for-service model, which provides hospitals and doctors incentive to prescribe more services, to the accountable care model, which compensates health care providers on a fixed basis to promote preventative care while removing the incentive for excessive and duplicate services.
“That is the transformation we are all moving toward,” Auger said. “It is incumbent on health care providers to help people stay healthier besides the fact it is just the right thing to do.”
Keeping people healthier will also provide breathing room for hospital and health care facilities suffering from a nationwide physician shortage and overwhelmed by patients streaming into emergency rooms for common ailments.
“I have heard as high as 70 percent of doctor urgent care and ER visits are unnecessary,” Auger said. “Costs are spiraling out of control. The focus of all health care systems now is to lower the cost of care.”
Just this year, Norwalk Hospital opened its new Bauer Emergency Care Center to specifically address the influx of patients coming into its emergency room for nonlife-threatening needs.
Prior to the opening of the center, Norwalk Hospital representatives said 70 percent of patients who visited the hospital”™s emergency room came for vertical care, meaning they were able to walk in and did not require a wheelchair.
With the uptake of St. Vincent”™s telemedicine initiatives steady, the hospital is now looking into pilot programs to expand virtual care to include video and areas such as cardiac monitoring and behavioral health, said Auger.
Within the Yale New Haven Health System, telemedicine initiatives and pilot programs are in use including video observation and consultation.
The system”™s longest running telehealth service is dubbed telestroke. It has been in service since 2008 and allows doctors to remotely view and prescribe treatment for stroke patients at the Yale-New Haven Hospital Stroke Center in real time.
The health system has pilot telemedicine services being tested and in development including a telepsych service.
Addressing the issue of cost, the health network has been using its telepsych service to find a solution to night and weekend staffing issues at one of its campuses by connecting patients via video-link to mental health professionals at another campus.
The health care provider is also bringing virtual care into its intensive care observation centers. Remote monitoring technology, including zoomable video, has allowed more patients to be observed and monitored by fewer staff and may be expanded to conduct follow-up observations with stable organ transplant recipients.
But while the use of technology is allowing for more efficient use of staff, it is not taking the place of staff, said Tara Estabrooks, the health system”™s associate director for business development.
“It isn”™t replacing the in-person types of interactions,” she said. “It is supplementing care.”
Beyond doctor-patient interactions, the ability to conduct videoconferences is allowing doctors to quickly confer simultaneously with multiple specialists and staff or allow far-removed family members to take part in medical discussions or simply console their hospital-bound relative, Estabrooks said.
Many of the programs are in the pilot or planning stages, but like Buccini, Patrick and Auger, Estabrooks said she sees today”™s telemedicine services as the early stage of a new evolution of modern medicine that will quickly advance alongside technology in the coming years.
From virtual reality examinations and bedside robots to 3-D printed devices and lab grown organs, the future of health care in the next decade or two may be far beyond what we can imagine today, Patrick said.
“I would say it is still in the early stages ”“ kind of like the internet circa 1996,” he said. “The advances in the next ten years will exceed what we have seen in the last 100 years.”