To explain the situations that New York Medical College”™s Center of Excellence in Precision Responses to Bioterrorism and Disasters will help address, Dr. Robert W. Amler said to picture the final scene of an action or disaster movie.
Sure, the hero has done what he set out to do and solved whatever crisis he faced, but in real life that would only be a small part of the story, said Amler. After all, plenty of people may have been harmed before our hero finally resolved or prevented the calamity.
“If you”™re a medical responder, your movie is just starting,” he said. “Because you know you have potentially hundreds of victims, even thousands, suddenly showing up for medical care.”
How to help those medical responders deal with a rush of victims in a stressful setting following a terror attack or natural disaster will be part of the focus for the Valhalla center, which the college officially opened on June 8. It will provide training for disaster and terror situations, as well as focus research on responses to chemical and biological terror threats.
The Center of Excellence designation comes from the state”™s economic development arm, Empire State Development. The state will provide a $500,000 initial grant to New York Medical College to help launch the center. There are currently 11 centers of excellence in New York state focused on a range of research topics, but this will be the first in the Hudson Valley, according to New York Medical College officials.
“The state wants to bring innovation technology into each region in a way that will stimulate more outside investment from the federal government and private sources,” Amler said.
Part of that innovation investment could come in tandem with New York Medical College”™s BioInc@NYMC life sciences incubator, which occupies a portion of the 120,000-square-foot building at 7 Dana Road that will primarily be used for Center of Excellence training. Amler explained that the center”™s research on strategies to combat biological and chemical threats could come from or help advance products from companies based at the incubator.
New York Medical College will also develop a full-time “austere medicine” training facility for training first responders. The space will be able to simulate the types of disorienting scenes ”” active shooter situations, fires, car accidents ”” that a first responder or physician could face while trying to provide care.
“Where there is smoke or fog that obscures your vision, where there”™s lots of loud noises going off and explosive noises that are both frightening and distracting,” Amler said of thjsoe simulated scenes. “Even the possibility of trained actors that can run through a scene panicky and disruptive.”
That”™s what Amler described as “the fog of war,” and he said it inevitably leads to mistakes. “But the kind of training Dr. Reilly provides, which is not based on protocols but principles, can make sure we don”™t repeat the same mistakes over again,” he added. He was referring to Dr. Michael J. Reilly, director of the Center for Disaster Medicine at New York Medical College.
The Center for Disaster Medicine previously has conducted this type of first responder training as part of a pilot program with the U.S. Department of Defense. The increased state funding that comes with being declared a Center of Excellence will help New York Medical College build out those training programs, which use military strategies to guide decisions by first responders in dangerous and dynamic environments.
“We”™re talking about doing things now to enhance the civilian emergency medical response to not just terrorism, but all types of disasters and public health emergencies,” Reilly said.
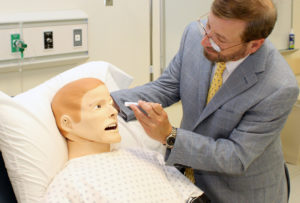
That training will incorporate some of the simulators owned by New York Medical College. They look like mannequins or crash test dummies but are far more complex. One type of simulator, which Reilly said costs from $75,000 to $90,000, can replicate basic human actions such as breathing and blinking and is operated through Wi-Fi to display symptoms and injuries.
Using state money, Reilly said the center will be able to purchase more of the simulators. That includes mechanical paitents built specific to trauma injuries, which can bleed – and bleed out – and offer more options for surgical procedures.
“We hope we can upgrade to better technology not only to train our students but all people that come here for medical education simulation training,” Reilly said.
The simulators were on display when New York Medical College officially opened the Center of Excellence at a ceremony on June 8. State Sen. Terrence Murphy, who helped secure the state grant, said at the ceremony that the center “gives the region a vitally needed local resource to fight terrorism and potentially protect the lives of first responders and our families.”
The main area where training and simulation will be staged is still undergoing renovations. Reilly said the college hopes to ramp up its emergency response programming by August.















